What is a stroke?
We have information and videos about What is a stroke? in other languages, including Arabic, Chinese (Cantonese & Mandarin), Greek, Italian, Macedonian, Turkish, Korean, Hindi, and Vietnamese.
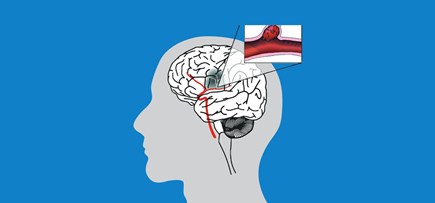
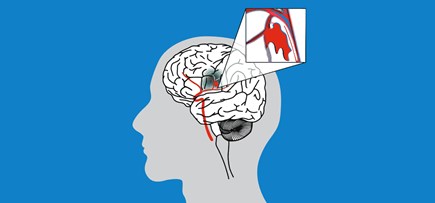
There are two types of stroke.
Both types of stroke stop blood getting to areas of the brain:
How does it affect people?
Stroke attacks the brain, the human control centre.
The brain is divided into areas which control different things. The impact of the stroke depends on the area of the brain it damages. Damage to an area of your brain can impact how you think, behave, use words, swallow, see, feel, touch, and move your body.
Stroke affects everyone differently.
Who is at risk?
Stroke can happen to anyone of any age.
Men are at greater risk of stroke and as we get older our risk increases.
In saying that, stroke is preventable for many. Some of the causes within our control include high blood pressure, being overweight, smoking, high cholesterol, a high intake of alcohol and diabetes.
-

Prevent stroke
Did you know more than 80% of strokes can be prevented? Reduce your risk of stroke with a health check and a healthy lifestyle.
Read more -

Transient ischaemic attack (TIA)
The signs of TIA are the same as for a stroke, but they disappear within a short time. After a TIA, your risk of stroke is higher.
Read more